Ultrasound assessment of residual gastric volume in older adults undergoing staged-bilateral total knee arthroplasty after consuming carbohydrate-containing fluids: a prospective observational study
Article information
Abstract
Background
We compared preoperative residual gastric volume (GV) between the first and second stages of total knee arthroplasty (TKA) in older adults after drinking carbohydrate-containing fluid 2 h prior to surgery.
Methods
In this study, 36 patients, aged > 65 years, scheduled for staged bilateral TKA with one-week interval, were enrolled. The patients consumed 400 ml of carbohydrate-containing fluid 2 h prior to surgery. Before the induction of spinal anesthesia, the gastric antral cross-sectional area was measured at the first and second TKA using ultrasound, and the residual GV was calculated. The primary outcome was the residual GV. Qualitative GV (grades 0, 1, and 2) and analgesic consumption after the first TKA were assessed as secondary outcomes.
Results
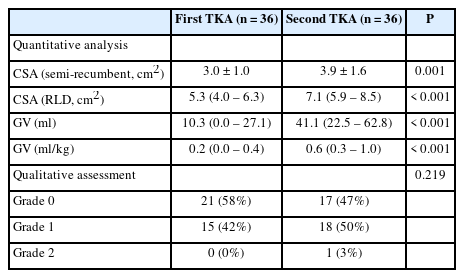
The GV (median [Q1, Q3]) was greater in the second-stage TKA (41.1 [22.5, 62.8] ml) than in the first-stage TKA (10.3 [0.0, 27.1] ml) (P < 0.001). In the qualitative assessment, the distribution was not different between the two stages of TKA (P = 0.219) and only one patient showed grade 2 gastric content in the second TKA. When opioid consumption was converted to an equivalent dose of morphine, an average of 53.9 mg of morphine was required after the first TKA.
Conclusions
Residual GV after drinking carbohydrate-containing fluid differed according to the stage of TKA, showing a larger residual GV in the second TKA than in the first one. In older adults scheduled to undergo bilateral staged TKA, caution is required in preoperative fasting practice, especially in second-stage surgery.
Introduction
Although modern preoperative fasting guidelines encourage the consumption of carbohydrate-containing fluid 2 h prior to surgery [1], it is debatable whether this practice is appropriate and safe in all patients undergoing various types of surgery [2,3]. One study demonstrated that fasting time was not associated with residual gastric volume (GV), showing that the incidence of full stomach was 35% in patients who had unplanned surgery and fasted for at least 6 h [4]. Even in scheduled laparoscopic cholecystectomy, 13% of patients showed a full stomach despite adherence to the recommended fasting time [5].
In our institution, many patients undergo staged bilateral total knee arthroplasty (TKA) at weekly intervals, most of whom are older adults with degenerative arthritis. As recommended, older adult patients who underwent TKA drank carbohydrate-containing fluid 2 h prior to surgery. In staged bilateral TKA, additional points should be considered when applying fasting guidelines. In addition to advanced age [6] that can affect gastric emptying time, the patient’s physical, medical, and psychological conditions may differ during the first and second operations [7]. For example, the effect of the acute pain after the first TKA and subsequent opioids use on gastric motility cannot be ignored [7,8]. However, to date, no studies have examined the residual GV of older adult patients with staged bilateral TKA and whether there is a difference according to the stage when carbohydrate-containing fluid is ingested.
Our hypothesis is that the preoperative residual GV of older adults drinking carbohydrate-containing fluid 2 h before surgery may be different between the first and second TKA. This study evaluated and compared preoperative residual GV measured using ultrasonography in older adults undergoing staged bilateral TKA.
Materials and Methods
This prospective observational study was conducted at Seoul National University Bundang Hospital between March 2021 and March 2022 according to institutional and Good Clinical Practice guidelines. This study complied with the 2013 Declaration of Helsinki. The study protocol was registered at ClinicalTrials.gov (NCT04814706, registered on March 24, 2021) after obtaining approval of the Institutional Review Board on March 16, 2021 (B-2103/673-302; Chairperson, Hak Chul Jang; Seoul National University Bundang Hospital).
The subjects were older adults (65 – 85 years) scheduled for staged bilateral TKA with one-week interval under spinal anesthesia. Patients with chronic kidney disease, diabetes mellitus, previous history of esophagus or stomach surgery, gastroesophageal reflux disease, and an American Society of Anesthesiologists physical status score > 3 were excluded. All patients provided written informed consent before participation.
The enrolled patients consumed 400 ml carbohydrate-containing fluid (Nucare NoNPO®; 12.8% maltodextrin, 50 kcal/100 ml, 0.52 mg/ml sodium, 0.48 mg/ml potassium; Daesang Wellife, Korea) 2 h prior to surgery. In addition, 75 mg of pregabalin, 200 mg of celecoxib, and 650 mg of acetaminophen were administered with sips of < 20 ml of water 1 h prior to surgery for pre-emptive analgesia.
Residual GVs were measured twice before the first and the second TKA by ultrasound. Ultrasound examination was performed in the preoperative holding area in a semi-recumbent and right-lateral decubitus (RLD) position for the greatest sensitivity [9]. A cross-sectional image of the gastric antrum was identified using a low-frequency convex array transducer (probe rC60xi, 2 – 5 MHz) equipped with an ultrasound machine (SonoSite EDGE II, Fusifilm SonoSite Inc., USA). The gastric antrum was evaluated according to a standard protocol [10].
Both quantitative and qualitative methods were used to assess the residual GV. Images of the gastric antrum taken between peristaltic contractions were used to calculate the cross-sectional area (CSA). The CSA of the antrum in the RLD was calculated using two perpendicular anteroposterior (AP) and craniocaudal (CC) diameters of the antrum (Fig. 1): CSA = π × AP × CC / 4.
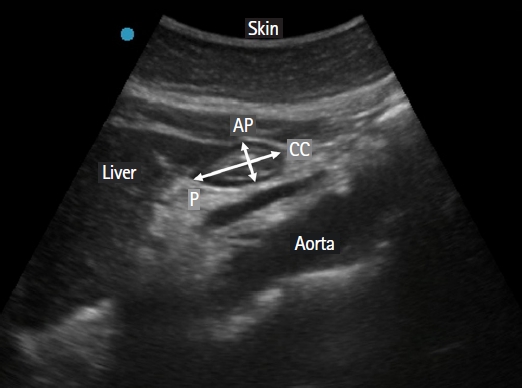
Ultrasound image of the gastric antrum in the epigastric area obtained in a sagittal or parasagittal plane. AP: antero-posterior diameter of antrum, CC: cranio-caudal diameter of antrum, P: pancreas.
CSA was measured three times and the average value of the three measurements was applied to the following formula to calculate the residual GV that was validated previously [11]: GV (ml) = 27.0 + 14.6 × RLD-CSA (cm2) – 1.28 × age (year). In the formula, RLD-CSA refers to the antral CSA measured in the RLD position. A calculated GV of less than zero was considered 0 ml.
Qualitative assessment was performed using a simple three-point grading system as defined by Perlas et al. [12]. Grade 0, completely empty antrum in both semi-recumbent and RLD positions; grade 1, empty antrum in the semi-recumbent position but visible fluid in the RLD position; grade 2, visible fluid in the antrum in both positions, implying a high-volume state.
Tramadol and morphine were administered for postoperative pain control. When the patient complained of a numeric rating scale score ≥ 4, 100 mg of tramadol was administered. Tramadol was administered up to four times a day, at least 4 h apart. When pain control was insufficient, as per the basic protocol described above, additional 5 mg of morphine was administered.
The primary outcome was the calculated GV. Qualitative assessment of GV (grades 0, 1, and 2) and analgesic consumption after the first TKA were included in the secondary outcomes.
Statistics
Sample size calculation was performed using G*Power software (ver. 3.1; Heinrich-Heine-Universität Düsseldorf, Germany). In our pilot study, the residual GV was 39.4 ± 39.1 ml prior to the first TKA. Considering that the 50% increase in the second TKA was statistically significant, 35 participants were required for an alpha level of 0.05 and a power of 80%. Assuming an overall loss to follow-up rate of 10%, a total of 39 participants were needed in the present study.
After a normality check using the Shapiro-Wilk test, paired t-test for CSA in a semi-recumbent position and Wilcoxon signed rank test for RLD-CSA and GV were used. For the comparison of qualitative assessment of GV (categorical data) between the two stages, the McNemar-Bowker test was used. Continuous variables are presented as mean ± standard deviation (SD) or median with interquartile range, and categorical variables are presented as numbers (proportions). Statistical Package for Social Sciences (SPSS; ver. 25; IBM Corp., USA) and Stata SE version 17 (Stata Corp., USA) software was used for the calculations, and all P values < 0.05 were considered significant.
Results
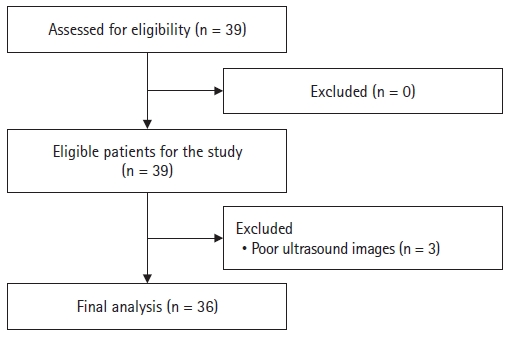
A total of 39 patients who were scheduled for staged bilateral TKA were enrolled in this study. Among them, three patients were excluded because of poor ultrasound images (Fig. 2). Patient characteristics are shown in Table 1.
Ultrasound evaluation of residual GV
The CSA measured in either the semi-recumbent or RLD position differed significantly between the first and second TKA (Table 2). Accordingly, the preoperative GV (median [Q1, Q3]) was significantly different between the first and second TKA (10.3 [0.0, 27.1] ml vs. 41.1 [22.5, 62.8] ml) (P < 0.001), and the mean difference in GV was 35.0 ml (95% CI [21.6, 48.5] ml). At the second TKA, a GV > 1.5 ml/kg, a criterion considered high risk for pulmonary aspiration [13,14] was observed in six patients. However, no patient presented pulmonary aspiration.
In the qualitative assessment, the distribution was not different between the two stages of TKA (P = 0.219) and only one patient showed grade 2 gastric content in the second TKA, whose calculated residual GV was 109.1 ml (1.6 ml/kg).
Opioid consumption
The amount of opioid consumption after the first TKA was also investigated (Table 3). Among the 36 patients, five did not require rescue analgesics for postoperative pain control. The mean doses (mean ± SD) of tramadol and morphine were 522.2 ± 434.9 mg and 1.7 ± 4.6 mg, respectively. When tramadol was converted to an equivalent dose of morphine, an average of 53.9 mg of morphine was required after the first TKA.
Discussion
This study found that the preoperative residual GV in the second TKA was greater than that in the first TKA when gastric ultrasonography was performed in older patients after consuming carbohydrate-containing fluid 2 h prior to each surgery. Previous studies have shown that preoperative carbohydrate intake in older patients does not change the gastric emptying time, residual GV, or gastric contents [2,15,16]. However, repeated surgeries that were performed at one-week interval increased the preoperative residual GV under the same fasting condition.
One notable aspect of this study was that residual GV > 1.5 ml/kg was observed in six patients before the second TKA operation that fortunately did not manifest as pulmonary aspiration. Although the strict threshold of GV that increases the risk of pulmonary aspiration is controversial, recent reports have announced that patients with GV > 1.5 ml/kg are a high-risk group for pulmonary aspiration [13,14], and residual GV > 1.5 ml/kg was occasionally observed in fasted patients suggesting incomplete gastric emptying [5,17]. However, there was a report that no one had a residual GV > 1.5 ml/kg after 2 h of drinking carbohydrate-containing fluid in ambulatory surgery [18], and in our study, there was no patient with a residual GV > 1.5 ml/kg in the first TKA. Further studies are needed to determine whether the same criteria should apply to patients taking carbohydrate-containing fluid before surgery and whether a residual GV > 1.5 ml/kg is appropriate to defer elective surgery for the prevention of pulmonary aspiration.
Various factors such as diabetes mellitus, chronic kidney disease, Parkinson’s disease, advanced age, and drug-induced gastroparesis have been known to be associated with delayed gastric emptying [19]. Among them, the effect of stress, especially emotional stress, on gastric motility is an ongoing debate and few studies have investigated the effect of surgery-induced stress on gastric emptying [20]. In the present study, since TKA was performed twice in one patient with one-week interval, stress caused by the first TKA was expected to affect gastric motility before the second TKA [21]. Unfortunately, the severity of patients’ stress was not measured using objective tools. Several tools, such as the Hospital Anxiety and Depression Scale [22], a brief measure of emotional preoperative stress [23], State-Trait Anxiety Inventory Form X [24], or a 10-items perceived stress scale [25], can be evaluated in future study. In addition, the levels of several stress biomarkers such as cortisol, interleukin-6, tumor necrosis factor-α, and C-reactive protein can be evaluated and compared.
Postoperative acute pain can be considered as one of the contributing factors for increased GV in the second TKA. Pain, a significant stressor [26], activates sympathetic reflex [27] and participates in the release of stress-related neuropeptides [28]. The sympathetic nervous system and neuropeptides have an inhibitory role over gastrointestinal muscle tone and motility, resulting in delayed gastric emptying [29]. Acute surgical pain added to chronic pain of the knee could influence the gastric emptying time, which might result in an increased residual GV before the second surgery [7,8].
Finally, the role of opioids used for postoperative analgesia should be considered. It is well known that opioid receptors are widely distributed in the body and play a critical role in various physiological processes, including immunological response, growth, and pain modulation [30]. In addition to these physiological processes, opioids play an inhibitory role in tonic/segmental contraction, peristalsis, and secretion in the gastrointestinal tract by binding to peripheral μ-opioid receptors, and consequently, intestinal propulsion is impaired and bowel transit time is delayed [30]. In the present study, most patients requested additional rescue analgesics during the rehabilitation period after the first TKA, and the mean dose of morphine equivalent was 54 mg. Since gastric emptying is suppressed even with a small dose of morphine [31], opioid analgesics administered after the first TKA may have contributed to the increase in residual GV before the second TKA. Unfortunately, however, our results did not show any correlation between residual GV changes and the amounts of opioid administered (R2 = 0.043, P = 0.804). Still interestingly, although there was no statistical difference, six patients with residual GV > 1.5 ml/kg showed more morphine equivalent dose (MED) than the others did (67.0 ± 46.5 mg vs. 51.3 ± 42.3 mg, P = 0.186).
Taken overall, this study could not identify a clear mechanism for why the residual GV was larger in the second TKA than in the first one. A larger well-planned trial is required to evaluate the correlation between the residual GV and opioid use or the severity of stress. Another limitation is that our results cannot be generalized to all populations, since the enrolled cohort consisted of older adults. TKA is a surgery mainly performed on elderly patients, so there would be no study conducted on younger patients in the same operation. It is necessary to perform a study on younger patients under similar surgical conditions. Last, the volume effect of water consumed for pre-emptive oral analgesic medication on the residual GV cannot be ignored. However, the allowed volume of water for oral medication was less than 20 ml. Furthermore, in some studies, the mean residual GV was approximately 37 – 83 ml even after 8 h of fasting before surgery [18,19]. Therefore, even if a small amount of water for oral analgesic medication is added to the residual GV identified as a result of this study, most of the cases do not seem to reach the GV amount observed in fasted people.
In conclusion, the residual GV differed according to the stage of TKA, with a larger residual GV in the second surgery than in the first. Hence, in older adults scheduled for bilateral staged TKA, caution is required when ingesting 400 ml carbohydrate-containing fluid 2 h before surgery, especially in the second surgery.
Notes
Funding
None.
Conflicts of Interest
No potential conflict of interest relevant to this article was reported.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Hyun-Jung Shin (Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Validation; Writing – original draft; Writing – review & editing)
Heeyeon Kim (Investigation; Methodology)
Sung-Hee Han (Conceptualization; Investigation; Methodology)
Sang-Hwan Do (Conceptualization; Methodology)
Hyo-Seok Na (Conceptualization; Data curation; Supervision; Writing – review & editing)