|
 |
| Korean J Anesthesiol > Volume 77(2); 2024 > Article |
|
Abstract
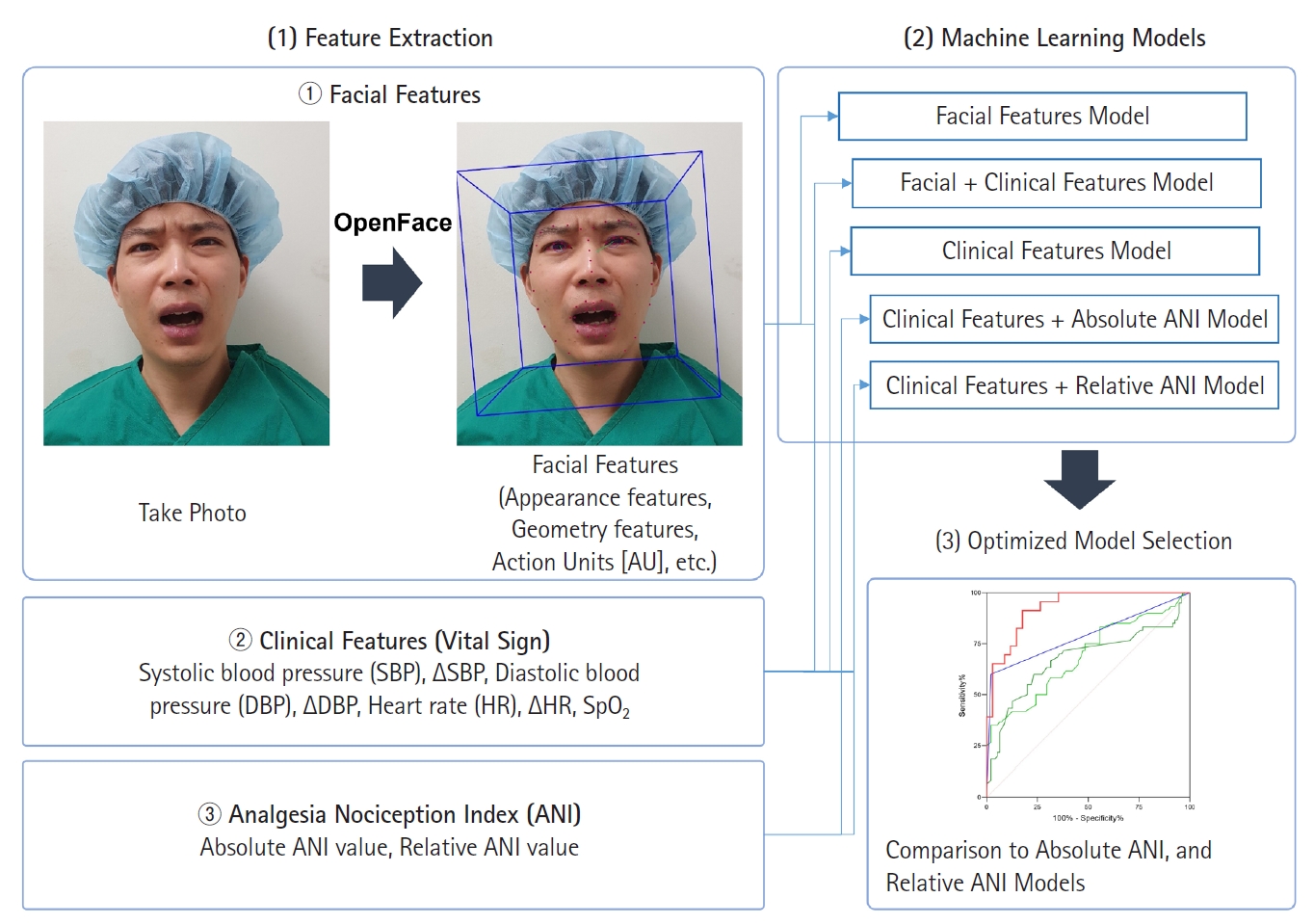
Background
Methods
Results
Acknowledgments
NOTES
Conflicts of Interest
Jung-Hee Ryu has been an editor for the Korean Journal of Anesthesiology (KJA) since 2018 and Bon-Wook Koo has also been an editor for the KJA since 2023. However, they were not involved in any process of review for this article, including peer reviewer selection, evaluation, or decision-making. There were no other potential conflicts of interest relevant to this article.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Insun Park (Conceptualization; Data curation; Formal analysis; Writing – original draft; Writing – review & editing)
Jae Hyon Park (Conceptualization; Data curation; Formal analysis; Methodology; Writing – original draft; Writing – review & editing)
Jongjin Yoon (Formal analysis; Methodology; Visualization; Writing – review & editing)
Hyo-Seok Na (Writing – review & editing)
Ah-Young Oh (Writing – review & editing)
Jung-Hee Ryu (Writing – review & editing)
Bon-Wook Koo (Conceptualization; Formal analysis; Methodology; Project administration; Supervision; Writing – original draft; Writing – review & editing)
Supplementary Materials
Supplementary Fig. 1.
Supplementary Fig. 2.
Fig. 2.
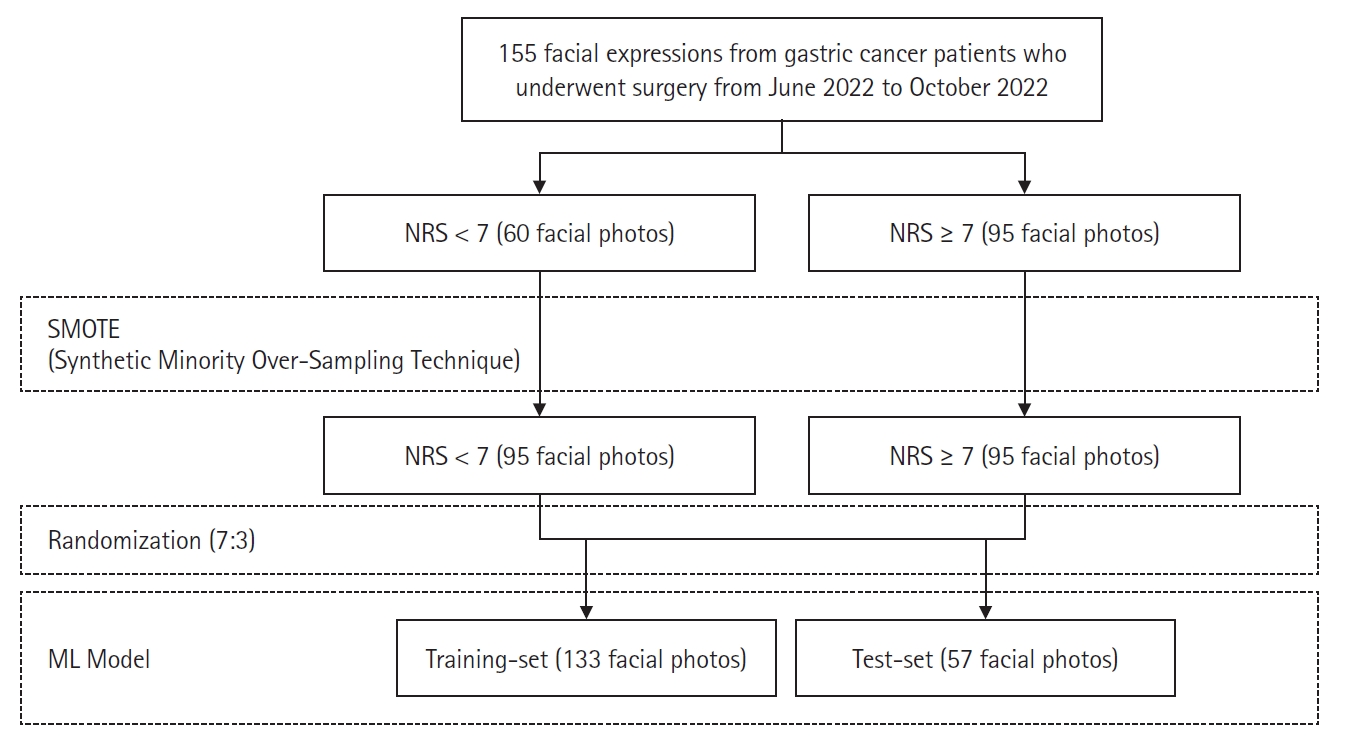
Fig. 3.
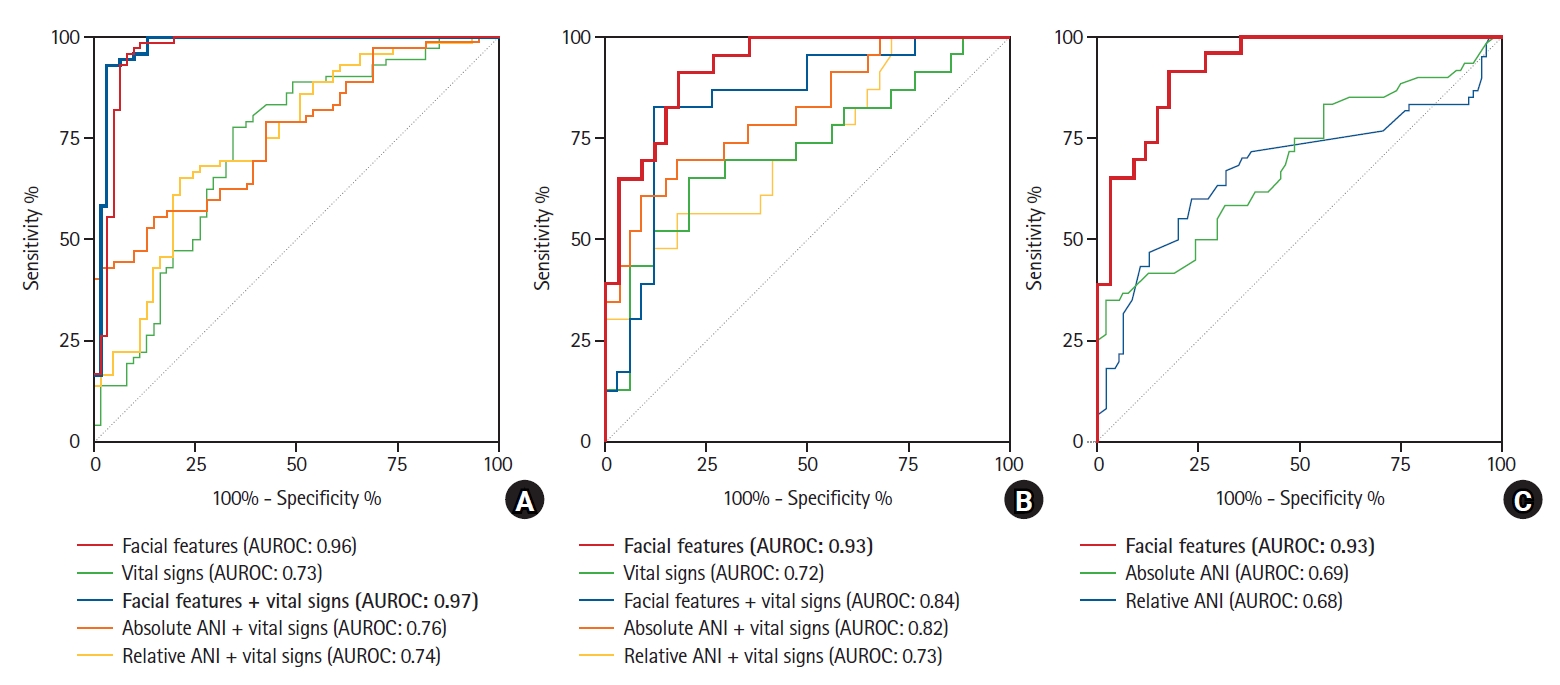
Table 1.
Table 2.
PPV: positive predictive value, NPV: negative predictive value, ML: machine learning, NRS: numerical rating scale, AUPRC: area under the precision-recall curve, AUROC: area under the receiver operating characteristic curve, ANI: analgesia nociception index. *P value was computed by comparing the AUROC of the model to the AUROC of the ‘facial features’ model via DeLong’s test.
Table 3.
PPV: positive predictive value, NPV: negative predictive value, ML: machine learning, ANI: analgesia nociception index, AUPRC: area under the precision-recall curve, AUROC: area under the receiver operating characteristic curve. *P value is computed by comparing two models (Absolute ANI [≤ 42], and Relative ANI [≤ −14]) to the ‘facial features’ model by DeLong’s test. †P value is computed by comparing Relative ANI (≤ −14) model to Absolute ANI (≤ 42) model by DeLong’s test.